 
Delay between PNH diagnosis and pregnancy was also recorded, as well as specific PNH treatment during pregnancy. Pancytopenia was considered when the 3 hematopoietic lineages were altered. Cytopenias were defined by 2 or 3 of the following criteria: anemia, defined as hemoglobin (Hb) levels less than 12g/dL thrombocytopenia, defined as platelet counts less than 150×10 9/L and neutropenia, defined as neutrophil counts less than 1.5×10 9/L. Dates of diagnosis and circumstances leading to diagnosis (presence of cytopenias, hemolysis, or thrombosis) were recorded. We analyzed maternal and fetal complications during pregnancy, delivery, and the postpartum period.Ī diagnosis of PNH was defined as an unequivocally positive Ham test before 1996 or by flow cytometry demonstrating the presence of more than 5% GPI-AP deficient polymorphonuclear cells after this time point. Here, we retrospectively reviewed 27 cases of pregnancy in 22 French women with PNH between 19. Venous thrombotic events (VTEs) were the major cause of maternal death. 4 Maternal and fetal mortality rates were 11.6% and 7.2%, respectively. Although there is little information about PNH and pregnancy in the literature, a recent review identified 23 clinical reports published between 19 describing pregnancy outcomes in 43 women with PNH. 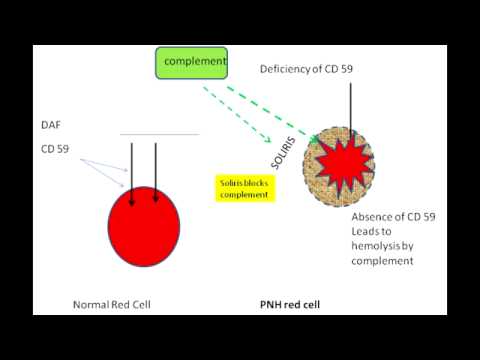
Worsening cytopenias may complicate the management of pregnancy but the main concern is the occurrence of thrombosis, which is responsible for the high mortality rates in pregnant PNH patients. Pregnancy in women with PNH is associated with an increased risk of complications for both mother and fetus, leading to high maternal and fetal mortality rates. A frequent association between PNH and aplastic anemia (AA) has been described, with 2 potential patterns of evolution: progressive marrow failure in PNH patients or AA in which a PNH clone is detected. 1 Patients are at risk for thromboses, major life-threatening risks of PNH, 2 which often occur at unusual sites. Patients with PNH may present with a wide range of clinical manifestations such as weakness, pallor, and asthenia due to hemolysis, but also abdominal pain, dysphagia, or pulmonary hypertension. 
Manifestations of the disease are primarily related to complement-mediated intravascular hemolysis due to the lack of glycosylphosphatidylinositol-anchored complement regulatory proteins (GPI-AP) CD55 and CD59 on erythrocyte cells. Paroxysmal nocturnal hemoglobinuria (PNH) is a rare, acquired, stem cell disorder characterized by hemolytic anemia, bone marrow failure, and venous thromboembolism. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
